What is TMVII?
Trichophyton mentagrophytes genotype VII (TMVII) is a fungal skin infection gaining attention within 2SLGBTQiA+ communities. While new to many in North America, staying informed about its symptoms and treatment will be a key part of maintaining community health.
The Health Initiative for Men (HIM) recently highlighted information regarding TMVII in their monthly newsletter, bringing attention to this easily treatable but currently little known infection. TMVII can look like ringworm, but if it’s appearing mostly around the groin area, it’s probably TMVII. In any case, it’s worth it to get checked out.
What is TMVII?
TMVII (say “TMseven”) is a sexually transmitted fungal infection. In 2023, doctors in Paris, France, first reported on an emerging fungal infection called TMVII (trichophyton mentagrophytes genotype VII) and cases were identified in the United States in late 2024. Data indicates that the majority of these cases occur among gay men and other men who have sex with men.
As a dermatophyte, this fungus thrives on keratin found in the skin. It is distinct from common ringworm because it specifically targets the groin, pubic, and buttock areas. It is also more persistent than typical fungal infections like athlete’s foot.
TMVII is primarily considered "anthropophilic," meaning it is adapted to spread between humans. Research and clinical reports, particularly those from outbreaks in Europe and the US, identify direct skin-to-skin contact—specifically sexual contact—as the main route of transmission.
What does it look like?
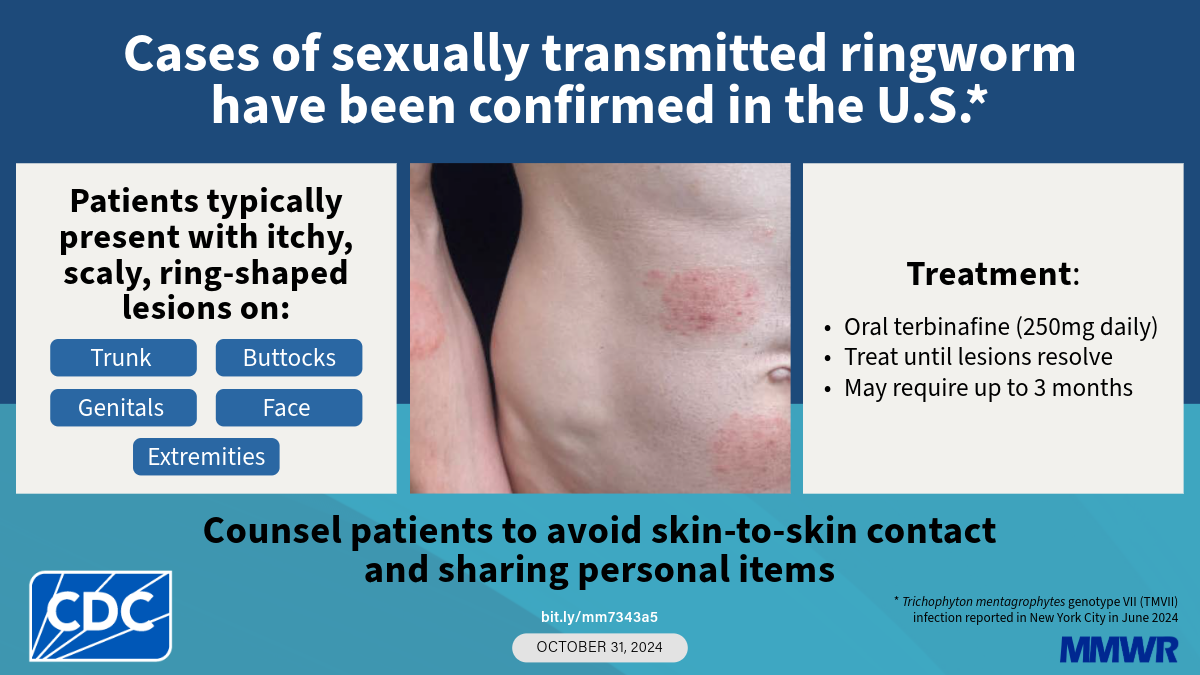
The symptoms of TMVII can easily be mistaken for other skin conditions, but there are specific characteristics to monitor:
Persistent Rashes: Highly inflamed, circular, and itchy rashes.
Lesions: Scaly or blistered lesions that resemble ringworm.
Location: These typically appear around the genitals, inner thighs, and buttocks.
Easily Treated - Get it Done!
Effective medical interventions are available, though they differ from standard over-the-counter treatments:
Oral Medication: Most common skin creams are insufficient for TMVII. Treatment typically requires oral antifungal medication, such as Terbinafine.
Consistency: A full course of treatment usually lasts between 4 to 6 weeks to ensure the infection is fully cleared.
Medical Oversight: Healthcare providers are monitoring this strain due to potential resistance to standard treatments in related fungi, though Terbinafine remains the primary effective option.
What if I don’t have a Doctor?
If you do not have a family doctor in British Columbia, several alternative pathways are available to ensure you receive a medical consultation for TMVII.
Dedicated 2SLGBTQiA+ Health Centres
For many in the community, dedicated health centres provide a safe and affirming environment for sexual health concerns:
Health Initiative for Men (HIM): HIM operates several health centres throughout the Greater Vancouver area that offer full-spectrum sexual health testing and primary care through nurse practitioners. You can book an appointment online or visit their Davie Street location for walk-in services.
Island Sexual Health (Victoria): This community health centre offers comprehensive sexual health care and STI management for people of all genders and orientations.
Sexual Health and Youth Clinics
Health authorities across BC run clinics that do not require a family doctor referral:
Vancouver Coastal Health (VCH): Clinics such as the East Van Sexual Health Clinic and Boulevard Sexual Health Clinic offer free, confidential STI testing and treatment for all ages.
Fraser Health Youth Clinics: If you are under the age of 25, you can access judgment-free sexual health care at various Youth Clinics throughout the Fraser Health region.
SmartSex Resource: This BCCDC tool includes a clinic finder to help you locate the nearest health centre or community clinic offering STI testing and treatment.
Primary Care Options
If you cannot access a specialized clinic, these general services are available:
Urgent and Primary Care Centres (UPCCs): These centres are designed for non-emergency health concerns that need to be addressed within 12 to 24 hours.
Your local pharmacist: While your pharmacist can’t prescribe the oral medication, many have telehealth access to doctors which they will share with you.
Walk-in Clinics: You can visit any walk-in clinic for an assessment; many offer same-day appointments or phone/video consultations.
Community Support and Navigation
HealthLink BC (8-1-1): You can call 8-1-1 at any time to speak with a nurse or a patient navigator who can help you find a local clinic or service provider.
Vancouver Primary Care Network:
Nurse Practitioners
In British Columbia, nurse practitioners (NPs) have the full legal authority to prescribe the medications used to treat TMVII, such as oral Terbinafine. Within the BC healthcare system, nurse practitioners are recognized as independent prescribers who can diagnose conditions and manage treatment plans. Many nurse practitioners work within 2SLGBTQiA+ affirming spaces, such as Health Initiative for Men (HIM) clinics, specifically to provide accessible sexual health care and prescriptions without the need for a family doctor.
If you are seeking treatment for TMVII, you can book an appointment with a nurse practitioner at a community health centre, an Urgent and Primary Care Centre (UPCC), or through a specialized sexual health clinic.
Readers in Vancouver can see all options through this Vancouver Primary Care Network
Because TMVII requires specific oral antifungal medication, it is important to see a healthcare provider who can provide a formal diagnosis and a prescription. Using general over-the-counter creams without a consultation may not be effective for this particular strain.
Community Care and Prevention
Prioritizing sexual health involves open communication and proactive care. Familiar prevention strategies remain the most effective tools:
Partner Communication: Discuss STI status and any new symptoms with sexual partners.
Symptom Awareness: Avoid sexual contact if you or a partner notice a new or developing rash.
Professional Consultation: Seek a healthcare provider immediately if you suspect symptoms. Delaying treatment can lead to skin scarring and other long-term effects.
Can I get it from my pet? TMVII is primarily considered "anthropophilic," meaning it is adapted to spread between humans. Research and clinical reports, particularly those from outbreaks in Europe and the US, identify direct skin-to-skin contact—specifically sexual contact—as the main route of transmission.
Can I spread it to my children
Highly contagious fungal infections like TMVII can pass to infants and children through both direct and indirect physical contact. Although the current spread among adults is primarily through sexual activity, a baby can contract the infection during routine care such as holding, cuddling, or skin-to-skin bonding if their skin touches an active rash. Additionally, indirect transmission occurs through shared items like towels, bed linens, or clothing, as the fungus can survive on surfaces for a period of time and infect a child who comes into contact with these materials.
Prevention Strategies for Parents and Caregivers
If you suspect you have TMVII, taking immediate steps to protect your child is essential:
Cover the Rash: Keep the infected area completely covered with clothing or a bandage at all times when around your baby.
Strict Hygiene: Wash your hands thoroughly with soap and water before picking up, feeding, or changing your baby.
Separate Laundry: Do not share towels or washcloths with your child. Wash your linens and clothes in hot water and dry them on high heat to help kill fungal spores.
Seek Medical Care: Visit a healthcare provider or a community clinic like HIM or Island Sexual Health immediately. Inform the provider that you have a young child at home so they can prioritize a treatment plan that reduces the risk of household transmission.
If you notice any new, circular, or scaly rashes on your baby, contact a pediatrician or visit an Urgent and Primary Care Centre (UPCC) right away. Early intervention is the best way to ensure the infection is managed safely for the whole family.
This is important:
The advice to seek a professional consultation rather than self-treating with pharmacy creams is the most important medical takeaway. Because this strain is persistent and can cause scarring if mismanaged, a formal diagnosis via a healthcare provider (at a clinic like HIM or a UPCC) is the necessary first step.